Occipital Nerve Stimulator (ONS) or Nerve Decompression Surgery
Take a look inside the differences between Nerve Decompression Surgery and Neuromodulation (Occipital Nerve Stimulator therapy & Peripheral Nerve Stimulator therapy). This information will help you understand the difference
How They Work
Nerve Decompression Surgery
(Dr. Carlton Perry’s approach)
This procedure directly addresses the mechanical root cause: inflammation and scar tissue that compress or entrap the occipital nerves, restricting blood flow (ischemia). The surgeon carefully releases the entrapped nerves and surrounding tissue without cutting the nerves themselves. This allows the nerves to revascularize—restoring normal oxygen and nutrient supply—so the ischemic pain signaling can quiet down naturally. It is a one-time, hardware-free surgery.
Peripheral Nerve Stimulation (PNS) / Occipital Nerve Stimulation (ONS)
Neuromodulation
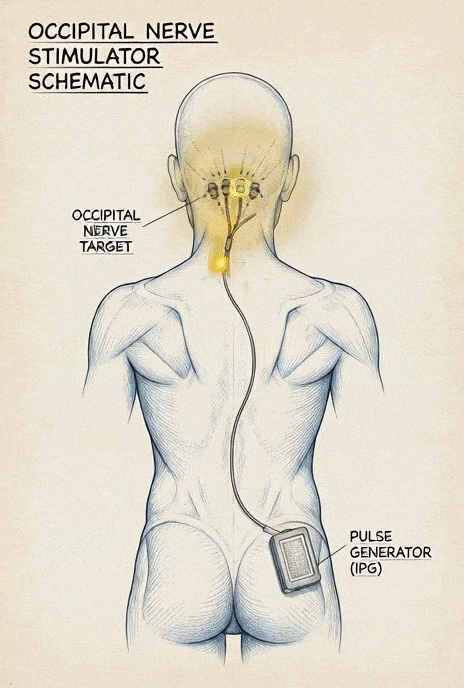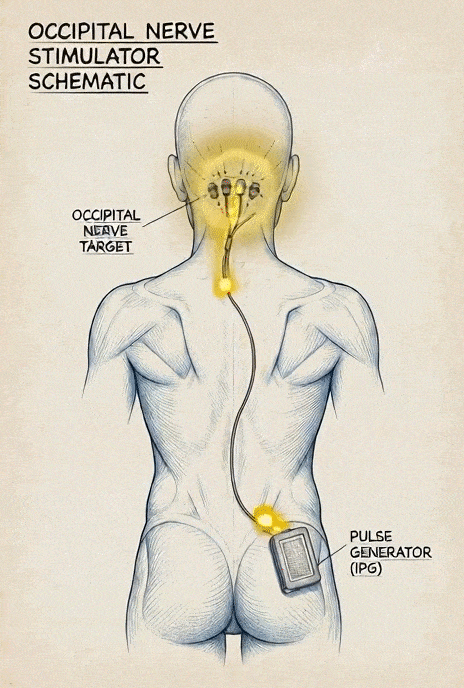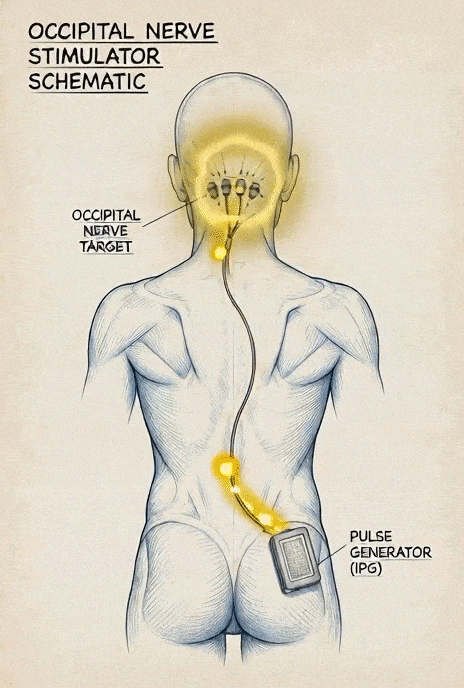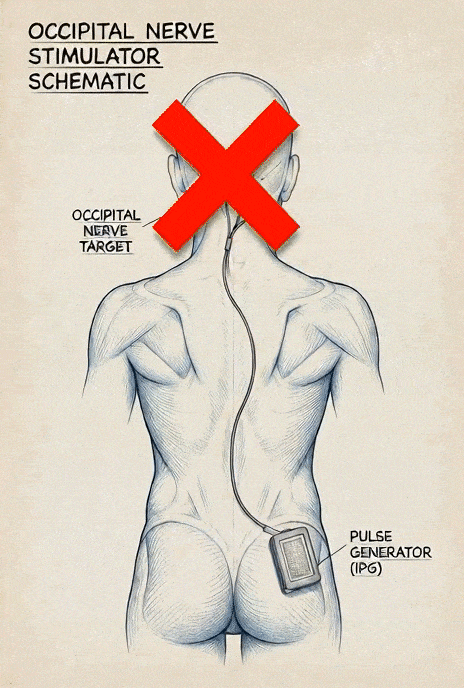
This involves implanting electrodes near the occipital nerves connected to a pulse generator. The device delivers electrical impulses that interfere with or “mask” pain signals traveling to the brain. It does not fix the underlying compression or restore blood flow—it modulates the signals after they are generated. Some systems allow a temporary trial before a permanent implant.
Ready to Take the Next Step?
Start the Free Pain Survey or call our office at 713.522.8228 to learn more. Patients have come from all 50 states and 12 foreign countries for this evaluation.
Where you go for nerve decompression surgery first truly matters — Dr. Carlton Perry does not cut nerves and performs immediate reconstruction if needed during the procedure.
Call our Houston office at 713-522-8228. We’re happy to answer your questions and help you figure out if this could be the right path for you.
Key Differences
Mechanism
Surgical Decompression treats the cause by releasing compression and restoring blood flow.
Neuromodulation treats the symptom by overriding pain signals electrically.
Hardware
Surgical Decompression is permanent and implant-free.
Neuromodulation usually requires a device (leads, battery/generator) that may need maintenance, replacement, or eventual removal.
Durability
Surgical Decompression aims for longer-term or durable relief by fixing the problem at the source.
Neuromodulation often provides good initial relief, but many patients experience fading efficacy over time. This fading is probably due to the progressive nature of the disease process, ongoing inflammatory tissue accumulation which causes more and more compression of more and more nerves, implanted device issues, and habituation.
Invasiveness and Maintenance
Surgical Decompression is a single surgery with typical recovery in weeks.
Neuromodulation involves implantation (and possible revisions) plus ongoing device management (battery changes, adjustments).
The proprietary pain survey, for head and neck pain is an industry leading game-changer in determining if our breakthrough pain relief procedures are right for your specific case.
Potential Benefits and Drawbacks
Nerve Decompression Surgery Benefits:
- Addresses the mechanical compression and ischemia directly.
- No implanted device, no battery replacements, no risk of lead migration, erosion, or infection from hardware.
- Nerve-preserving technique (does not cut nerves; immediate reconstruction if damage is present).
- Potential for more sustained relief once blood flow is restored.
Neuromodulation Benefits:
- Can sometimes be trialed temporarily before committing to a permanent implant.
- Less destructive than older ablative procedures (like nerve cutting or various types of ablation procedures).
- May help patients who are not good surgical candidates or who prefer a reversible option initially.
Nerve Decompression Drawbacks:
- Requires a skilled surgeon experienced in peripheral nerve work.
- Not everyone is a candidate (proper evaluation is essential).
- Surgical risks exist (as with any procedure), though the nerve-sparing approach helps minimize certain complications.
Neuromodulation Drawbacks:
- Does not resolve the underlying compression or ischemia, so pain can return or worsen over time.
- Common issues include lead migration, skin erosion, infection, battery depletion, and loss of efficacy.
- Many patients eventually need additional procedures or device removal.
Nerve Decompression Surgery Benefits:
- Addresses the mechanical compression and ischemia directly.
- No implanted device, no battery replacements, no risk of lead migration, erosion, or infection from hardware.
- Nerve-preserving technique (does not cut nerves; immediate reconstruction if damage is present).
- Potential for more sustained relief once blood flow is restored.
Nerve Decompression Drawbacks:
- Requires a skilled surgeon experienced in peripheral nerve work.
- Not everyone is a candidate (proper evaluation is essential).
- Surgical risks exist (as with any procedure), though the nerve-sparing approach helps minimize certain complications.
Neuromodulation Benefits:
- Can sometimes be trialed temporarily before committing to a permanent implant.
- Less destructive than older ablative procedures (like nerve cutting or various types of ablation procedures).
- May help patients who are not good surgical candidates or who prefer a reversible option initially.
Neuromodulation Drawbacks:
- Does not resolve the underlying compression or ischemia, so pain can return or worsen over time.
- Common issues include lead migration, skin erosion, infection, battery depletion, and loss of efficacy.
- Many patients eventually need additional procedures or device removal.
Don't Stop Others From Enjoying You.
We have developed an extensive protocol to help us determine which patients might have these issues and would be the best candidates for possible nerve decompression surgery for headache.
Which Might Be Right for You?
Nerve Decompression Surgery
Decompression surgery is often a thoughtful root-cause option for patients who have grown frustrated with medications or injections that don’t seem to reach the nerves effectively, or with stimulators that lose effectiveness over time. It appeals especially to those who want to avoid hardware and repeated interventions long-term.
Neuromodulation
Neuromodulation can still be helpful for some people (for example, as a temporary bridge or when surgery isn’t suitable), but patients who experience diminishing returns with it frequently explore decompression as a hardware-free alternative.
Important Note
This is not medical advice, and individual results vary. Neither approach is a treatment for classic episodic migraine (though some patients have overlapping conditions). The best way to determine what might help your specific situation is a thorough evaluation.
If you are dealing with occipital neuralgia (ON), chronic daily headache (CDH), or new daily persistent headache (NDPH) and feel like you’ve run out of effective options, take Dr. Carlton Perry’s Free Pain Survey or call our office at 713.522.8228. It includes an extensive interview and interactive 3D anatomical modeling to help assess whether nerve decompression surgery may address the compression-related component of your pain.
Start the Free Pain Survey or call our office at 713.522.8228 to learn more. Patients have come from all 50 states and 12 foreign countries for this evaluation.
Where you go for nerve decompression surgery first truly matters — Dr. Carlton Perry does not cut nerves and performs immediate reconstruction if needed during the procedure.
Occipital Neuralgia
(ON)
We have developed an extensive protocol to help us determine which patients might have these issues.
New Daily Persistent Headache (NDPH)
The exact cause of NDPH is still unknown, some medications and therapies can help manage the symptoms.
Chronic Daily Headache
(CDH)
Chronic Daily Headache is a debilitating and potentially life changing process. Our goal is to try and look for the source of the problem and correct it.
